It might seem simple, but it’s true that washing your hands with just water and soap kills germs like the flu, and coronaviruses such as COVID-19. Doing this, along with one or two other safety practices, you can do a lot to keep others around you from becoming sick if you have the flu, a common cold… or COVID-19.
While you may be wondering why hand washing is so much better than using hand sanitizers, you must realize that each of these has their place in the prevention of communicable illnesses. To kill coronavirus germs most efficiently, soap and water are the best weapons you have. Soap works to permeate the outer “skin” of the virus, which is made up of fat. Water alone doesn’t do this - you also need the soap, which helps to physically inactivate the coronavirus. When water and soap are not available, hand sanitizer is a good substitute.
About 70% of people wash their hands after using the bathroom; the remaining 30% don’t. About 15% of those who do wash after using the bathroom don’t do it correctly. You should be scrubbing your hands together briskly with soap, getting every area of the hand and fingers before rinsing and drying using a clean towel. There’s a handy image you can follow below if you’re a visual learner.
Resources for Before and After College
How Illnesses Spread
Different illnesses spread in different ways. The flu, for instance, can be spread person-to-person, from about 6 feet away. It spreads when someone who is sick with flu sneezes, coughs, or talks. The virus is contained in microscopic droplets that float in the air and land on hard surfaces or within the noses and mouths of other people. When someone touches a hard surface that has droplets of flu virus on it, then they touch their eyes, nose, or mouth, their chances of being infected with the flu rise exponentially.
Someone with the flu is most contagious three to four days after they become ill. However, a healthy adult can infect others one day before becoming sick and five to seven days after they have become sick. If someone has a weakened immune system, or they are a child, they may pass the virus on for more than seven days after getting sick.
If you have been close to someone who is sick with the flu and you haven’t taken any precautions, such as not touching your face or eyes, you are highly likely to develop the same illness. People with lung conditions are the most at risk to develop severe conditions from the flu—distance yourself and wash your hands.
When it comes to the newer COVID-19, it takes longer for those infected to show symptoms, up to 14 days. And it turns out that you can be contagious for an extended period of time before symptoms show, and for up to a full week after they appear. This, along with the excessive amount of infectious virus found in infected individuals, is likely a large part of the reason this virus has spread so quickly and so far.
Hand Washing
Washing your hands with warm water and soap is one of the best things you can do for your health and that of others around you. Specifically, you need to wash your hands after or before the following actions:
- After using the bathroom
- After caring for someone who is vomiting or has diarrhea
- After changing diapers or helping a child who has just used the toilet
- After cleaning up pet waste, touching a pet, or feeding them
- Before you begin cooking, as you are cooking, and afterward
- Before you eat
- After you cough, sneeze, or blow your nose
- After handling garbage
- Before you clean and treat a wound and afterwards
If you’ve never been given a step-by-step for the hand washing process, or there’s someone you think needs to know, this is for you:
- Wet your hands with warm, clean water that is running from the faucet. Lather your hands with soap and turn the water off.
- Lather your hands by rubbing them together briskly. Scrub the backs of your hands, in between your fingers, under your nails, and your palms. Scrub briskly for 20 seconds at minimum (to keep track, you can sing or hum “Happy Birthday” twice).
- Turn the water back on and rinse your hands well, then dry with a clean towel or paper towel.
If you need to wash your hands, but have no running water or soap, hand sanitizer can be a good substitute. Again, rub hour hands briskly together, on all surfaces, until the sanitizer has dried.
Hand Washing Illustration

Hand Sanitizer
Washing your hands with water and soap actually kills the germs residing on your skin. You’ll lessen the overall number of germs, including coronavirus and the flu, as you wash.
However, if you have no choice but to use a hand sanitizer, you should make sure you use one that has at least 60% alcohol by concentration. Any lower than that and it won’t be very effective. The Centers for Disease Control and Prevention (CDC) advocates for using water and soap any time you have it available.
While hand sanitizer is good when it’s necessary, it won’t kill certain types of germs, such as norovirus or Clostridium difficile. And, to kill the viruses it does work on effectively, you need to use the right amount and do so correctly. This usually means using more than you think is necessary and leaving it on your hands until it has dried.
If your hands are greasy or visibly dirty, hand sanitizer is not going to work effectively. In these situations, it’s worth it to go out of your way to find soap and water.
Coughing and Sneezing
Even if you know you are only suffering from allergies or asthma, you must still cover your mouth when you cough or sneeze. If nothing else, this will get you into the habit of covering your mouth before you get sick. That will make it second nature to cover your mouth and nose when you are actually ill.
Illnesses like COVID-19, the flu, and the common cold are spread by sneezing, coughing, and touching your face after touching something that has been contaminated. This means that covering your nose and mouth with a facial tissue when you sneeze or cough will be the most effective way of preventing the spread of illness. If you don’t have a tissue, you can cover your nose and mouth with the inside of your elbow. You should certainly cover these with nearly anything other than your bare hands, unless you plan on washing your hands every single time you cough, and I don’t think any of us have enough time for that.
Of course, the most definitive way of keeping from infecting anyone else is to stay home if you are sick. Or, if illness is moving through your community or office, you can choose instead to socially distance yourself.
Staying Home When Sick
Let’s say you’re sick, maybe you have the flu or COVID-19, which is caused by the coronavirus. Do you stay at home to rest or do you go to your classes or work?
The easy answer is that you should stay at home. If you go to school or work, you run a high chance of infecting others—and some of those people may have underlying health issues such as asthma, immunosuppressed systems, or other health issues that can make catching any illness dangerous. This is one of the same reasons we vaccinate. There are children and others who, due to congenital disorders, a past cancer diagnosis, or even allergies, cannot take vaccines and have compromised immune systems.
Even if you think you can stay away from your co-workers or other students, it’s possible that simply breathing may help to spread a virus spread through the air. If you breathe out through your mouth, the virus, which is suspended in tiny particles, can stay in the air for minutes to several hours, according to a new study.
Even if the particles are large and end up falling to a surface, someone could still be infected if they come into contact before the virus dies and then touch their own nose or eyes. If someone is standing close to you and you sneeze or cough, infected droplets can land in the noses or mouths of those people and they end up infected. As you can see, the risk is high no matter how you conduct yourself in public.
Social Distancing
Social distancing is defined as maintaining a 6-foot (2 meter) distance between yourself and another person. You’d also stay away from large gatherings because there’s no way to know if anyone you’re with is infectious or not. Remember, this is especially true with the new coronavirus, which someone can have and be contagious long before they show any symptoms. It doesn’t matter if everyone seems healthy, they could still infect new carriers to take home to their children, pets, and elderly relatives. That’s why many states are asking people to stay away from stadiums, large classrooms, movie theaters, malls, and more.
Social distancing also works when you are already sick. You’ll keep the infection from spreading among your family, friends, and fellow students. If you are determined by a medical professional to have COVID-19, you may be asked about close contacts. These are people who have been within 6 feet of you for more than just a few minutes while you were likely contagious. This means anyone you shared a waiting room or living space with while you were sick.
Face Masks
Face masks: a good idea or bad? It may be comforting to have something between you and possible contagion, but unless you’re a healthcare worker, then the truth is that you likely aren’t aware of the proper use of masks. Most people know how to use a simple dust mask to keep themselves from breathing in large particles, but if you are trying to protect yourself from illness it’s a whole other matter. Professionals use N95 masks to filter out tiny particles in the air. However, they often use thinner masks to maintain the cleanliness in a surgical room or around very ill patients.
When you wear one of these masks, it may keep out some small particles, but it won’t work well for long. As you breathe, you exhale warm, moist air. The longer you wear one of these masks, the more moist it becomes from your breathing—and the less effective it becomes at protecting you from any viruses floating around you.
This is part of why it is so important for medical professionals to have a stock of personal protective equipment (PPE). They cannot simply continue using a single mask indefinitely, and neither should you. Professionals really should be using N95 masks, but surgical masks are a good backup. The only reason you should ever worry about wear a mask is if you are feeling ill and have no choice but to leave your home. This can keep you from sneezing onto your hands, surfaces, or other people, making it easier for you to refrain from making anyone else ill.
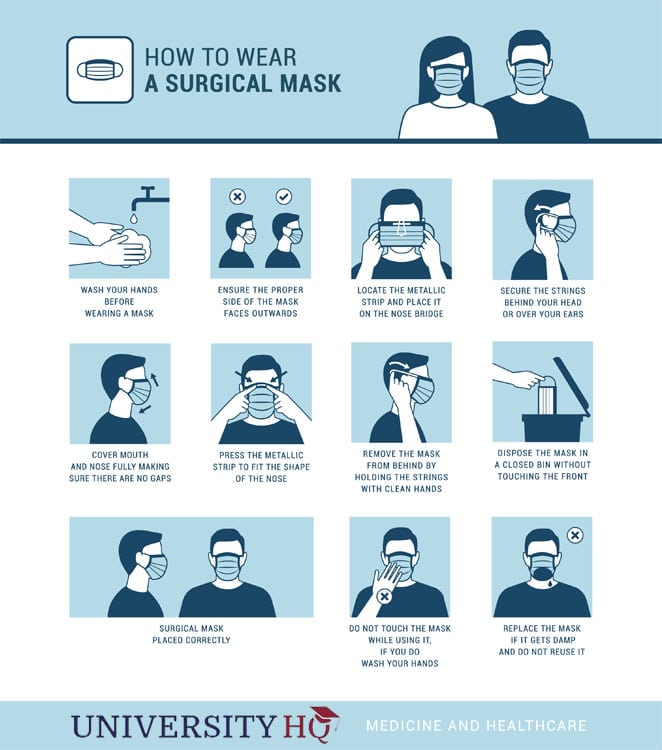
Why These are So Important During a National Crisis Like COVID-19
What is it?
COVID-19 is a strain of coronavirus that began to spread in people beginning in December 2019. Its symptoms are a high fever, tiredness, a dry cough, and difficulty breathing though before respiratory symptoms emerge it may present as gastrointestinal distress, headaches, and others. It looks very like the common flu. People with underlying health conditions are the most vulnerable to more severe symptoms. Symptoms may begin any time between two and 14 days after being exposed.
Where did it Come From?
This coronavirus, which has never been seen before, originated in Wuhan, Hubei province, China. It is a potentially severe respiratory disease that has since spread around the world and been classified as a pandemic.
The World Health Organization (WHO) was informed about this coronavirus on December 31, 2019 (thus the name COVID-19). Research has linked this illness to the same family of coronaviruses that have causes MERS and SARS, and the virus itself is actually called SARS-CoV-2. There are a variety of other coronavirus’ we are familiar with, including those that cause the common cold, but the virus that causes COVID-19 is more aggressive and more deadly.
Why is this Virus/Disease so Dangerous?
Even if people have told you, “It’s just like the flu”, it’s important to remember a few facts. First, at this point, COVID-19 is the direct cause of death in about 3.5% of those who become infected. The flu kills .1% of those it infects. Those with the flu are contagious for 2-3 days before symptoms begin, while those with COVID-19 could be contagious for over a week before they know they are sick. This affects the number of people that are likely to be infected by a single carrier; with the flu that number is 1-1.3, while those with COVID-19 could infect up to 2.5 people each.
These are the things that make COVID-19 so dangerous, what makes it a threat to everyone is the real possibility that healthcare systems around the world are likely to be overwhelmed by the numbers of patients with this disease. Countries like Italy and Spain are struggling to contain the outbreak. And, even if you do not catch it, or are not at risk of dying, overrun healthcare systems lead to a significant number of deaths among those not suffering from the cause. If you are in an auto accident but there are no trauma nurses available because they became sick with COVID-19, you may die. If you need to be put into a medically induced coma to recover from burns, but there are no ventilators available, you may die.
Medications and treatments that are viable, mass producible, and effective have yet to come to light and, even worse, a vaccine is at least a year, maybe 18 months, away.
How is it Spread?
COVID-19 is spreading rapidly, threatening to overwhelm cities, countries, and hospitals. While it’s a new illness, research has already revealing that it is spread from person to person in much the same way as the flu. This includes inhaling respiratory droplets from an infected person, between people who are in close contact (less than 6 feet or 2 meters apart), and possibly those in enclosed spaces together, such as an office.
It appears that people who have been infected, but who are not yet sick, are contagious, with spread taking place without their knowledge. However, someone who is sick with COVID-19 is the most contagious. This is why people are being asked to self-isolate or self-quarantine.
The worst part about this virus is that it is so easy to infect someone else, and community spread is already showing that the spread is highly sustainable. Community spread means that people have been infected without knowing where or how they got infected making it nearly impossible to track the spread or the “chain” of spread in order to target our quarantine efforts.
As of March, all 50 states were reporting cases of COVID-19. These include infections acquired through close contact with an infected person, illness that was imported by travelers, and community-acquired cases. Three states in the US are reporting sustained community spread. Because of this, some states are ordering shelter-in-place or stay-at-home orders for their residents.
Total Cases in the United States
As of March 25, 2020, the number of cases in the US reached 59,966. This included Puerto Rico and the District of Columbia. Clusters of outbreaks have been reported in Washington state, New York, and California with smaller clusters reported in many states.
Because our testing was rolled out more slowly than some countries, it’s difficult for local health departments and the CDC to know precisely how many cases there are on a given day. In New York state alone, more than 30,800 people have become ill (March 25). In New Mexico, this number is over 100, with most cases concentrated in the northern part of the state.
Nursing homes and assisted living facilities, which house a much higher number of those who are particularly vulnerable, have been hit especially hard. While seasonal flu still kills anywhere between 12,000 and 61,000 people annually, COVID-19 shouldn’t be dismissed as being “just like the flu”.
Who is Most at Risk?
Those who are at the highest risk of developing COVID-19 include healthcare workers who are taking care of patients with COVID-19. Travelers who are returning from international locations affected by the coronavirus are also at high risk, especially if community spread has begun in those countries. Those who have had close (less than 6 feet or 2 meters) with persons who were later found to be infected with COVID-19 are also at higher risk of developing this virus.
Older adults (over age 60), patients with HIV or any immune deficiency, those with diabetes, those who have or have had a cancer diagnosis, and people diagnosed with asthma or other lung conditions are at an elevated risk for a more severe case of COVID-19. And, while these are the people who are at the highest risk to die, it’s a fact that a significant number of those who are hospitalized are under 60 and even children have died because of this illness.
Moving to Online Classes
School districts and universities all across the US have cancelled all in-person classes; instructors have moved instruction to online platforms and standardized testing requirements have been waived. Some students may have thought that this was overkill, but research has since proven teachers and schools to be right. Not only do some students have underlying health conditions that make social distancing (and social isolation) a necessity for them to maintain their current level of health, but keeping them out of school will also mean there are fewer cases needing hospitalization.
People everywhere, students included, need to distance themselves from each other. In classrooms bursting with large classes, this is physically impossible. To deter the rapid spread of COVID-19, schools like Harvard, Berkeley, the University of Washington, Columbia, NYU, Duke, Barnard, Princeton, and more have cancelled all in-person classes. Some universities even made the controversial decision to close their dorms, requiring students to either go home or find off-campus accommodations.
Because of this, many students in elementary, middle, high school, and college are going to school 100% online. The change isn’t easy. However, schools and universities are taking this approach because they are responsible for protecting the health of their students.
Due to bans on travel (to international locations, particularly), international spring break travel and study-abroad programs have been canceled. Instead, study-abroad programs have been postponed to a time when international travel is safer; conferences take place virtually or are outright cancelled.
Though there are some issues in the way these changes were rolled out, and there are gaps and divides that will need to be addressed, these changes are good overall for those who want to maintain their health and still complete their education.
sources:
- https://www.medicalnewstoday.com/articles/why-hand-washing-really-could-slow-down-an-epidemic#Implementing-targeted-hygiene-campaigns
- https://www.cnn.com/2020/03/24/health/soap-warm-water-hand-sanitizer-coronavirus-wellness-scn/index.html
- https://www.cdc.gov/flu/about/disease/spread.htm
- https://www.cdc.gov/handwashing/when-how-handwashing.html
- https://www.cdc.gov/handwashing/show-me-the-science-hand-sanitizer.html
